Do I need a Knee Assessment?
Is it important that I see a doctor or physical therapist for a knee assessment? What will they ask me, and what will they look for?

Is it important that I see a doctor or physical therapist for a knee assessment? What will they ask me, and what will they look for?
USE the OMH exclusive code "HEALTH15" to Save 15%As a physiotherapist, I so often get a call from someone asking “What is wrong with my knee, because it is so sore and I do not know why?
And so I attentively listen to their symptoms and ask whether something has happened to their knee to cause the pain, and then most often I still land up saying something along the lines of “It could be various conditions, so the best would really be for you to come in and see me for a proper knee assessment so that I can give you a more accurate diagnosis and we can come up with a treatment plan specially designed for you…”
Why is it important to see a health care practitioner?
So although this article will give you some helpful and important information, it is almost always best to also consult a physical therapist, doctor or orthopaedic specialist in order to get a proper diagnosis. These medical professionals will ask you some important questions and do the necessary examinations in order to give you an accurate diagnosis.
In order to prepare you for your visit to your health care practitioner, here is a list of the sorts of questions you may be asked. So you can give it some thought before you go, and remember that honesty is always the best policy!
Questions your health care practitioner will ask you during your knee assessment
- What age are you? This gives an idea of the sorts of conditions you may be suffering from. A 20 year old is very unlikely to have osteoarthritis, but may well have anterior knee pain.
- What is your current level of activity? An ultra-marathon runner will have more likelihood of overuse and wear and tear conditions than a walker.
- Has anything happened that you think may have caused your knee pain? A specific injury will definitely affect different structures compared to non-injury related pain, which seems to have started gradually or out of the blue.
- How long have you had your knee pain? This gives an idea of whether the pain is acute or chronic, and affects the chosen treatment.
- Is it getting better, getting worse, or staying the same? This gives the medical practitioner an idea of the “stability” of the condition, and whether it may be easily flared up.
- What makes your knee pain worse? And what makes your knee pain better? This gives an idea of what sort of condition it may be – for example osteoarthritis is worse after periods of being in one position for too long, while an acute ligament injury would definitely feel better being kept still.
- Have you got any other joint problems? Additional joint issues may also point to a possible systemic problem if more than one joint is affected.
- Do you have any medical conditions such as thyroid issues, cardiovascular problems, diabetes, cancer etc? This information would give the health care practitioner additional clues as to possible systemic problems, or contributing factors.
- Are you on any medications? It is important for the health care practitioner to know because sometimes medications can cause side effects, or may adversely interact with other medications which he or she may prescribe.
- What is your weight and height? Your body-mass index (really your weight related to your height) should ideally be between 18.5 and 24.9. If you are overweight or obese, this will place more stress and strain on your joints, and unfortunately predispose you to developing certain conditions such as osteoarthritis.
It is really important to answer these questions as accurately and as honestly as you can. They give the health care practitioner plenty of useful information in order to be able to help you get better.
Examinations your health care practitioner will perform
The doctor, or physical therapist will firstly look at your knees to see if there are any visible signs of the following, and compare them to the other side too:
- Swelling – is the one knee slightly puffy, or even massively swollen?
- Redness – this may be a sign of inflammation or infection
- Changes in muscle size – the muscles around the knee joint sometimes get smaller (atrophy) in response to an injury
- Bony changes – there may be noticeable differences in the bony appearance, and these may point to a chronic condition (such as osteoarthritis)
- Is the knee slightly bent, or even over extended – these also give the practitioner clues as to what may be going on in your knee joint.
The practitioner will then gently feel your knee joint in order to discern where the pain is felt. This gives important clues as to which structures are involved – whether it is a ligament, your meniscus or the fat pad, which is affected. Perhaps you have trigger points (painful tender spots) in the muscles around the knee joint?
Physical tests and ligament stability tests for a knee assessment
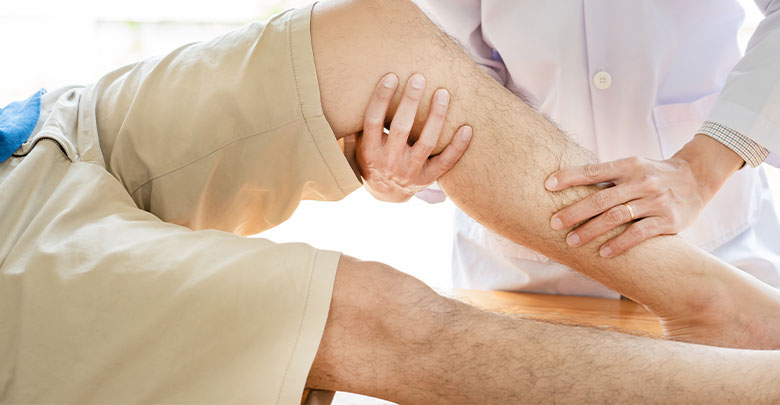
There are also numerous physical tests and ligament stability tests which the health care practitioner will perform.
- He or she will check what your range of movement is in your knee – by simply asking you to bend and straighten your knee as far as you can. The practitioner may also move your knee for you in order to check your passive range of movement.
- While doing these movements the practitioner will notice the quality of the movement – is it stiff, grinding, clicking or clunking?
- You may be asked to lift your leg, or perform a few simple exercises so that your muscle strength can be gauged.
- The ligament tests check the stability of your anterior cruciate ligament, posterior cruciate ligament, medical collateral ligament and lateral collateral ligament. The practitioner will be able to feel if there is excessive movement in these ligaments, or whether the test reproduces pain – which may point to a tear in that ligament.
- He or she will probably move your patella around gently to check for tenderness behind the knee cap, which can be an indication of inflammation behind the knee cap; tenderness below the knee cap, which is the area of the patella tendon; to the sides of the patella below the knee cap are the fat pads; and above the knee cap over the quadriceps tendon.
Further knee assessment examinations
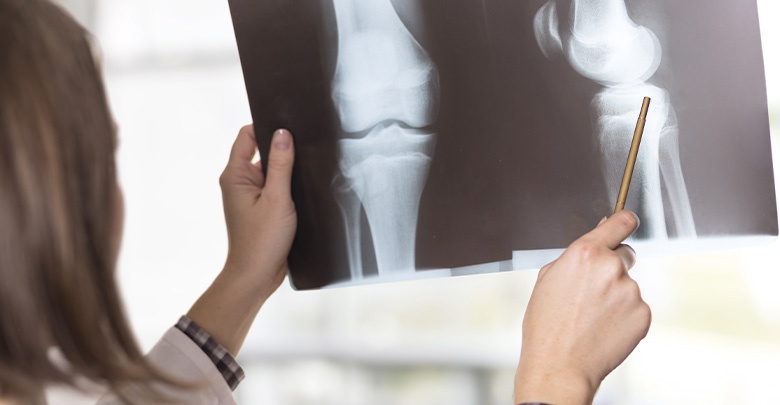
So after all these questions, and having your knee thoroughly looked at and moved around, your health care practitioner may have a very good idea of what exactly is going on. Sometimes further examinations are needed. These may include
- X-rays of your knee joint – these are important to be able to see the bony structures of your knee, to get an idea of whether the joint spaces are normal, and to see if there are any bony fragments. However issues may get missed on x-rays.
- Ultrasound scans – these scans are relatively inexpensive to perform, and some practitioners have the equipment in their consulting rooms. Ultrasound scans are useful in order to image fairly superficial (close to the surface) injuries of the knee joint.
- MRI scan – an MRI scan is usually an expensive investigation, and so it is only required when it is essential to get images of the ligaments, menisci, joint capsule and muscle tissue (all the “soft tissues” which do not show up on x-rays). These MRI scans do not always show everything that there is to be seen though, in which case it may be necessary to undergo arthroscopy
- Arthroscopy – sometimes, it may be necessary for an orthopaedic surgeon to insert a tiny camera into your knee to have a proper look at the internal structures of the knee. Often the doctor will take the opportunity while he is looking inside, (if he has your express permission) to fix any meniscal, ligamentous or minor cartilage defects while he has you under anaesthetic.
- Blood tests – if the doctor suspects that you may have a condition such as gout, rheumatoid arthritis, or some sort of inflammatory condition, you may have to have blood tests done. There are over 200 different kinds of arthritis alone, and blood tests play an important role in getting an accurate diagnosis if any of these sorts of problems is suspected.
As you can see, it is impossible to get an accurate diagnosis without seeing a health care practitioner. It is also good to know that anyone you see should really give you a thorough knee assessment as described above, in order to get an accurate diagnosis.
A proper diagnosis is the first step to managing your injury or condition. From there you can manage your symptoms, start an appropriate strengthening and rehabilitation programme, make the lifestyle changes necessary to prevent deterioration, and ensure a healthier, happier you. So be kind to yourself. Be kind to your joints!